Patient Education
Colon Polyps
What is a colon polyp?
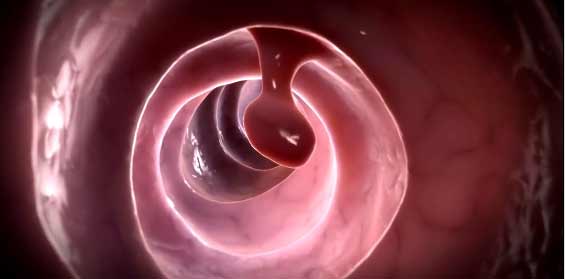
A colon polyp is a small lump that forms on the lining of the colon (large intestine). There are several types of colon polyps, including some that can turn into colon cancer. However, the majority of colon polyps are harmless. Most colon polyps don’t cause symptoms, but removal is usual during a colonoscopy for cancer prevention and testing.
Types of Colon Polyps
There are two main types of colon polyps: non-neoplastic and neoplastic. Non-neoplastic polyps are less likely to become cancerous and include hyperplastic, inflammatory, and hamartomatous polyps. Neoplastic polyps include adenomas, the most common type of pre-cancerous polyps.
Adenomas have the possibility of becoming cancerous in the future, and the risk of colon cancer increases as the polyp grows larger.
Regular screening tests, like a colonoscopy, are important. Finding and removing colon polyps early is the key to preventing colon cancer.
Important facts about colon polyps:
- They’re common. 30 to 50 percent of adults will develop colon polyps
- Not all colon polyps turn into cancer
- It takes years for a polyp to turn into cancer
- Polyps can be removed safely and completely
What Causes Colon Polyps?
The exact cause of colon polyps is unknown, but it appears lifestyle and environmental factors make an impact.
Lifestyle
Several lifestyle factors increase your risk of developing colon polyps.
- High-fat diets
- Diets high in red meat
- Low-fiber diets
- Smoking cigarettes
- Drinking alcohol
- Obesity
Age
Those 50 and above are more likely to develop colon polyps, which is why doctors recommend screening for colon cancer at age 50. If you have a family history or other risk factors of polyps, your doctor may recommend screenings at a younger age.
Race
African Americans are more likely to develop colon cancer, and screening may be recommended before age 50.
Family History of Colon Polyps & Genetics
Genetic factors are important since polyps and colon cancer tend to run in families. If a family member has had colon polyps or colon cancer, it’s important to talk with your doctor. This is especially true if the family member is immediate and/or developed colon cancer at a young age.
Those with a family history of colon polyps should begin colon cancer screenings earlier than 50.
In rare cases, people inherit genetic conditions that make them more likely to develop polyps and colorectal cancer. These include:
Familial adenomatous polyposis (FAP) – a rare disease that can cause many polyps to form as early as teenage years. Without treatment, the risk of colon cancer is nearly 100% before the age of 40. Genetic testing can help determine your risk for FAP.
Hereditary Non-Polyposis Colon Cancer (HNPCC) – Also known as Lynch Syndrome, this disease increases the risk of developing colon cancer in your 20s and 30s. It does not cause a large number of polyps, but the polyps that do form can become malignant much faster. Among the inherited disorders, Lynch Syndrome is the most common. It is associated with tumors in the ovaries, urinary tract, small intestine, stomach, and breast.
Genetic testing is available for patients at high risk or family history of colon cancer but isn’t recommended for patients at normal risk for colon cancer.
Colon Polyp Symptoms
Most colon polyps don’t cause symptoms, and most patients won’t know they have polyps until they have a colonoscopy. Because there are no symptoms, it’s important to keep a regular screening schedule.
Some may experience:
- Pain – Polyps that are large could obstruct your bowel and cause abdominal pain or cramping.
- Rectal bleeding – Blood may be present after a bowel movement or found in your underwear. This can also be due to small tears in your anus or hemorrhoids.
- Stool color change – Blood can make your stool look black or have streaks of red. This could also be from certain foods, drinks, or supplements.
- Change in Bowels – Constipation or diarrhea lasting a week or more.
Colon Polyp Diagnosis
Since most colon polyps will not have symptoms, many are detected for the first time during a screening for colon cancer like a colonoscopy. The ways colon polyps are usually detected include:
- Colonoscopy: A long flexible tube with a camera is placed through the rectum and into the large intestine. This allows the doctor to see any polyps and remove them at the same time.
- Sigmoidoscopy: Less invasive but limited in scope, this procedure allows the doctor to view the lower third of your colon using a small lighted tube. If polyps are found, a colonoscopy will be necessary to remove them.
- CT/Virtual Colonoscopy: This test is minimally invasive and uses a CT scan to inspect your colon. Bowel preparation for a virtual colonoscopy is the same as a regular colonoscopy, and a colonoscopy will be necessary if polyps are found.
- Stool tests: Patients provide a stool sample that tested for blood and assesses stool DNA. Patients with a positive stool test will need a colonoscopy.
Colon Polyp Removal
Colon cancer is preventable if polyps are found and removed before turning into cancer. When doctors find colon polyps they will remove them and send them for testing. This eliminates colon polyps’ ability to turn into cancer. Polyp removal is painless because the colon does not have the ability to feel pain. Most are found and removed during a colonoscopy.
- Polypectomy: The medical term for removing polyps. The majority of polypectomies are done with a colonoscope, the device used to perform a colonoscopy. Small polyps are snipped and the tissue removed. Slightly larger polyps are removed using a wire loop that cauterizes the removal site and prevents bleeding.
- Laparoscopic Surgery: In rare cases, polyps too large to remove during a colonoscopy will require minimally invasive surgery.
- Removal of Colon / Rectum: In rare cases of inherited diseases like FAP, your doctor may recommend complete removal of your colon and rectum. This is called a total proctocolectomy.
Once removed, your polyps will be analyzed by a tissue sample expert (pathologist). This evaluation will help determine your risk for developing colorectal cancer.
Complications with removal – Polyp removal is safe but still carries a risk of complications. The most common complications include perforations (creating a hole in the large intestine) and bleeding. Bleeding is generally controlled during a colonoscopy using cauterization.
After colon polyp removal
If your polyps are found to be adenomatous or serrated your risk of cancer is higher. The risk level is determined after examining the characteristics and size of the polyps. You will need follow-up exams to look for new polyps.
There is a 25 to 30 percent chance that adenomatous polyps will be found on a colonoscopy done three years after the initial test.
Your doctor will help you determine what screening schedule is right for you based on your results.
Colon Polyp Prevention
Screening for colon polyps and removing them during a colonoscopy is the standard procedure to prevent colon cancer. While polyps may not be preventable, you can lower your risk by:
- Eating more vegetables, fruit, and fiber
- Avoiding foods high in fat
- Losing extra weight
- Avoiding smoking and alcohol
Family Implications
Because of the hereditary nature of colon cancer and colon polyps, your family should be made aware of adenomatous polyps or colon cancer.
A first-degree relative (FDR) is a parent, brother, sister, or child.
- Those with one or two FDRs with colorectal cancer or adenomatous polyps before age 60 should begin screenings earlier. Typically this means screenings begin at age 40 or 10 years younger than the earliest diagnosis – whichever is sooner.
- Those with one FDR with colorectal cancer or adenomatous polyps at age 60 or later should start screenings at 40 years old. If no polyps are found, it should indicate an average risk and typical screening guidelines apply.
- Those with a grandparent, aunt, uncle, great-grandparent, or cousin with colorectal cancer should be screened similarly to someone of average risk.
Colon Polyp Testimonials
“I turned 50 this year and as a part of my commitment to take better care of myself, I treated myself to a colonoscopy. I’m generally in good health and was really just ‘checking the box on this (so I thought). During the exam, Dr. Garza identified and resolved a serious issue that typically serves as a precursor to cancer. He is kind, compassionate, and extremely good at what he does. His staff was amazing and I can’t thank them enough for helping me.” – MC
“Dr. Hearne was very thorough in a recent visit, both informative in general and specifically explaining the two kinds of precancerous colon polyps, one of which hardly ever becomes cancerous. Needless to say, I was also pleased to learn that the type of polyp found so far in my own colon was not the kind that sometimes further develops into cancer. Dr. Hearne taking some additional time to educate me and his easy-going manner are both winners. He is my gastroenterology doctor going forward.” -Dennis
“Dr. Garza has taken great care of me. I am a colon cancer survivor. Colon cancer runs in my family, and Dr. Garza answers my questions and calms me. He has a great bedside manner. I highly recommend Dr. Garza. AND remember an ounce of prevention is worth a pound of cure. Don’t miss your colonoscopy, prep is not fun, BUT sitting in a chemotherapy drip room is REALLY not fun. Trust me!!” -Susan