Hemorrhoids: An Ultimate Guide
What are hemorrhoids?
Hemorrhoids are swollen, enlarged veins in your rectum or around your anus. They are most often caused by pressure on the veins, like the kind of pressure caused by straining to push out a bowel movement. You may have heard them called piles.
Hemorrhoidal tissue is a normal part of our anatomy. It is thought to help cushion muscles when having a bowel movement and hold stool in when we are not. We usually don’t notice hemorrhoids unless they become swollen.
Hemorrhoids are a very common condition that becomes more common with age. Most everyone will have hemorrhoids at some point but may not have noticeable symptoms. It’s estimated that half of all people over 50 have noticeable hemorrhoids.
Women often get hemorrhoids during pregnancy, but they tend to clear up after childbirth.
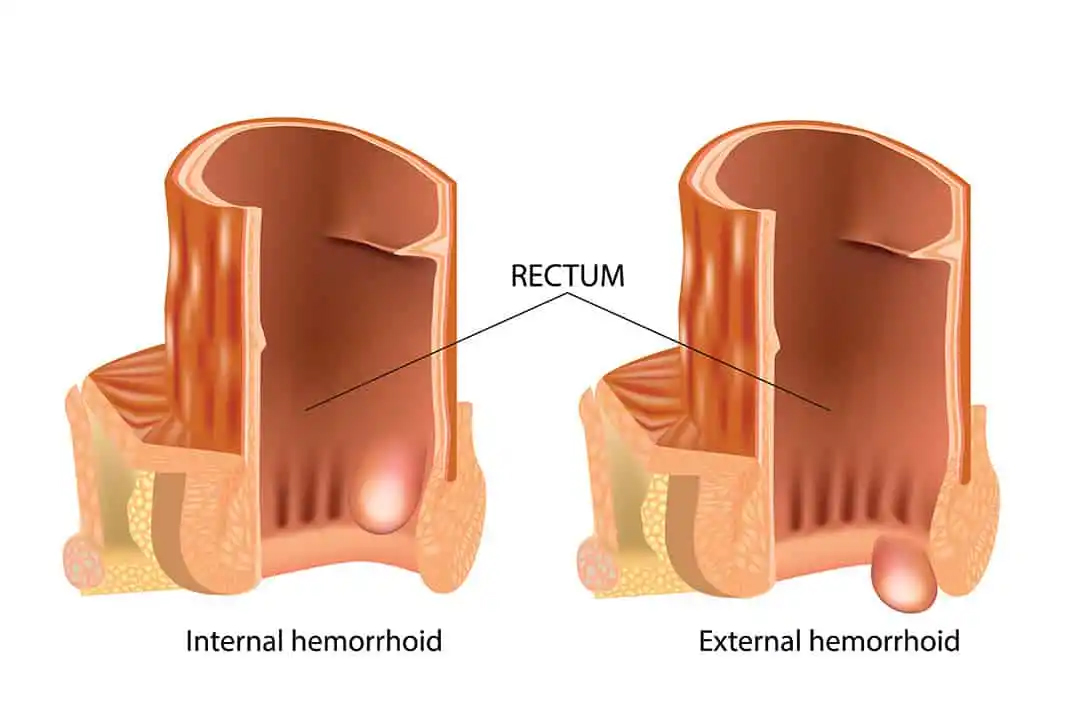
There are two main types of hemorrhoids:
- Internal – Hemorrhoids that are inside the rectum. They are usually not noticeable.
- External – Hemorrhoids in the tissue around the anus.
When hemorrhoids occur, they often become more of a problem if they are thrombosed or prolapsed.
Thrombosed – An internal or external hemorrhoid that has formed a blood clot, called a thrombosis, that can be felt and seen in the skin around the anus. They develop hard lumps and may be purple or blue. They can cause further inflammation and can be very painful.
The blood clot in a thrombosed hemorrhoid can’t travel to other areas of your body, like some other types of blood clots can. Removing the clot in the first 48 hours can provide the most relief, so it is important to call your doctor right away if you are experiencing sudden anal pain.
Prolapsed – Hemorrhoids that stretch and bulge outside the anus are called prolapsed. They can bleed and may be painful. A prolapsed hemorrhoid can become so swollen that it interferes with your ability to have a bowel movement. In rare cases, they can bleed severely enough to be dangerous. It’s essential to contact your doctor about any rectal bleeding.
What causes hemorrhoids?
Hemorrhoids can be caused by anything that puts pressure on the veins in and around the rectum and anus. Your risk of developing them increases as you age.
Common causes are:
- Sitting for too long
- Straining with bowel movements
- Chronic constipation or diarrhea
- Obesity
- Pregnancy
- Regular, heavy lifting
- A diet lacking fiber
- Anal intercourse
- Liver disease
- Family history of hemorrhoids
Hemorrhoid Symptoms
Symptoms can be different depending on the type, but it is possible to have more than one type. Once swelling causes itching, it can trigger a cycle of symptoms. Scratching, cleaning the area, or not cleaning well enough can cause even more itching. The itching can then lead to more bleeding and irritation.
Internal hemorrhoids are generally not noticeable unless they prolapse out of the anus. They may also cause noticeable bleeding if the veins get scratched or broken because of straining or itching. If you have bleeding from hemorrhoids, you may notice blood in the bowl, on the toilet paper, or in your stool.
External hemorrhoids may cause:
- Irritation
- Itching
- Pain or discomfort
- Protrusion or hard lump near the anus
- Rectal bleeding
- Swelling around the anus
Prolapsed hemorrhoids may cause:
- Pain or discomfort
- Bulging that you can feel outside the anus
Diagnosing Hemorrhoids
Some of the symptoms of hemorrhoids can be caused by other, more dangerous conditions, like colon cancer. If you’re having symptoms, it’s important to talk to your healthcare provider to rule out other causes. Your symptoms and a physical exam might be enough to diagnose hemorrhoids, but you may need other tests.
Physical exam – Your doctor will examine the anus and rectum for signs of hemorrhoids. Your doctor may need to feel inside the rectum.
Digital rectal exam (DRE) – Your doctor may check for internal hemorrhoids by inserting a gloved, lubricated finger into the rectum.
Anoscopy or proctoscopy – Your doctor inserts a small, lighted tube into the anus and rectum to examine the lining for symptoms.
Sigmoidoscopy – Your doctor inserts a small, lighted tube with a camera (sigmoidoscope) to assess the lower colon and rectum. The sigmoidoscopy can also be used to take a tissue sample for a biopsy if needed. A sigmoidoscopy can be done in the office with only an enema for preparation.
Colonoscopy — You may have a colonoscopy to confirm the results of other tests or to look for signs of colon cancer. A colonoscopy requires taking medication to empty the bowel and is done under anesthesia.
Home Remedies
Mild symptoms can often be treated successfully at home with lifestyle changes and over-the-counter medications. It’s important to get a diagnosis before starting any treatment, especially if you have bleeding or have never been diagnosed with hemorrhoids before.
Eat high-fiber foods
Having enough fiber in your diet helps soften your stool. Soft stool is easier to pass without putting extra pressure on your veins. Fruit, vegetables, whole grains, and legumes are healthy, natural sources of fiber.
Most adults should eat between 20-35 grams of fiber every day for healthy digestion, along with 6-8 glasses of water. If you don’t eat enough fiber now, you may need to increase your fiber intake slowly to avoid feeling gassy.
Fiber supplements
Over-the-counter fiber supplements are also an option if you can’t get enough fiber from food. They are safe to use every day with or without food. They can contain psyllium seed (like Metamucil®), methylcellulose (like Citrucel®), or calcium polycarbophil (like Fibercon®).
Although supplements are a good source of fiber, they can cause uncomfortable side effects like gas, bloating, and stomach cramping. If you decide to begin taking a fiber supplement, it is best to begin slowly so your body has time to adapt.
Good personal hygiene
Keeping the anal area very clean can help prevent and treat hemorrhoids. Clean gently after every bowel movement with soft toilet paper moistened with water. Too much wiping can irritate the area, especially with rough toilet paper. Using a squirt bottle, shower, bidet, or even a bath afterward can be less irritating than excessive wiping. Be sure to dry the anal area well.
Hemorrhoid Cream
Over-the-counter hemorrhoid creams, ointments, or suppositories that contain hydrocortisone may offer temporary relief from itching, pain, and inflammation.
Warm Sitz Bath
Bathing your anal area in warm water several times a day can help relieve hemorrhoid pain. A bathtub or a sitz bath are both good options. A sitz bath is a special tub that sits over your toilet that allows you to sit in several inches of water. Soak in a tub or sitz bath for 10-15 minutes, 2-3 times daily, especially after bowel movements.
Laxatives
Using laxatives may help ease constipation that can lead to straining and putting pressure on your hemorrhoids.
Pain Relievers
Over-the-counter pain relievers, like ibuprofen (Motrin, Advil) or acetaminophen (Tylenol), can temporarily help with pain or discomfort.
Use a step stool
Putting your feet on a small step stool during bowel movements changes the position of your rectum and may relieve your symptoms temporarily.
Minimally Invasive Treatments
Home remedies for hemorrhoids may not always work completely to relieve pain or other symptoms. Hemorrhoids that bleed too much or that have prolapsed need to be removed. Some removal procedures can be done in the office.
Hemorrhoid banding
Hemorrhoid banding, also called band ligation, is a non-surgical procedure that uses a special applicator to pinch the base of the hemorrhoid in a small rubber band. This restricts the blood supply to the hemorrhoid. The banded hemorrhoid will shrink and fall off during a bowel movement within a few days.
The procedure is quick, painless, and performed in the office. It only takes a few minutes, and you can return to your normal activities immediately. This option is only for internal hemorrhoids.
Endoscopy
Your doctor will insert a thin, flexible tube into your rectum. The tube has a tiny camera and can be used with small tools to remove hemorrhoids. Common methods are freezing, using infrared light, or electrical or laser heat.
Laser, infrared, or bipolar coagulation
These procedures use infrared light, heat, or a laser to shrink hemorrhoids. After treatment, the hemorrhoids will harden, shrivel, and eventually fall off.
Sclerotherapy
Sclerotherapy is an injection of a chemical solution into a hemorrhoid, causing it to shrink and form a scar.
Hemorrhoid surgery
If home treatment and minimally invasive office treatments don’t provide relief, your doctor may recommend a hemorrhoidectomy. This is a surgical procedure that removes the excess tissue that causes bleeding. It has a 95% success rate but can be painful.
The procedure is done under general or spinal anesthesia. Complications can include bleeding, bladder infection, or difficulty emptying the bowels or bladder. You may need to take pain medication during the recovery period.
When to see a doctor
In many cases, hemorrhoids can be treated successfully at home, especially if you’ve dealt with hemorrhoids in the past. But some circumstances need more than home remedies.
Call your doctor if:
- Pain lasts more than a few days or is severe
- Home remedies aren’t giving you relief
- You also have a change in bowel habits
- You have a fast-developing hemorrhoid or one that is very painful, which may have a blood clot (thrombosed)
- You have rectal bleeding
- You feel a lump
Go to urgent care or the emergency room if:
- You have a large amount of bleeding or bleeding that won’t stop
- You have bleeding with dizziness or lightheadedness
- You have anal pain that spreads, comes with fever, chills, or anal discharge, or gets progressively worse
Prevention
The best “treatment” for hemorrhoids is prevention. Taking steps to keep stool soft and to avoid the need to push or strain during bowel movements is the best way to prevent hemorrhoids. Here’s what you can do at home to help prevent hemorrhoids.
Stay hydrated
Drinking plenty of water and other healthy fluids throughout the day can help soften stool, making it easier to pass.
Eat fiber
Eating enough fiber every day can help soften stools and increase bulk, reducing the need to push and strain. Fruits, vegetables, whole grains, and beans are good, healthy sources of fiber. If you don’t normally eat much fiber, add it into your diet slowly to avoid feeling gassy.
Most people should get 20-30 grams of fiber per day. If you don’t get enough fiber in your diet, over-the-counter fiber supplements are the next best choice. When taking fiber, always drink plenty of water. Taking fiber without enough fluids can cause or worsen constipation.
Don’t strain
It can be frustrating to feel constipated, but straining to force stool out can cause hemorrhoids.
Go when you need to
Try not to wait too long to have a bowel movement when you feel the urge. When stool remains in your colon for too long, it can dry out and become harder to pass.
Keep moving
Regular exercise helps keep your gastrointestinal system moving. It can also help you maintain a healthy weight. Carrying extra weight can contribute to hemorrhoids. Even walking every day can help.
Don’t sit for long periods
Sitting too long at home or work, or on the toilet, can increase pressure around the anus, leading to hemorrhoids.
Hemorrhoids during pregnancy
Hemorrhoids can often occur during pregnancy, most often in the third trimester, during childbirth, or soon after. Nearly fifty percent of pregnant women will get them.
Hemorrhoids during pregnancy are caused by:
- Larger veins caused by the increased blood volume
- Pressure on veins from the growing uterus and baby
- Hormonal changes
- Constipation
They will usually disappear as the woman’s body returns to its pre-pregnant condition.
Treatment during pregnancy
It’s important to talk to your doctor before using any treatment that contains medication, even ointments or creams. Some home remedies include:
- Using wipes or hemorrhoid pads containing witch hazel
- Using flushable wipes after bowel movements
- Soaking in a tub or warm sitz bath for 10 minutes, several times per day
- Taking a bath or sitz bath with Epsom salts
- Using ice packs to soothe the discomfort
- Not sitting for long periods
- Doing Kegel exercises
- Resting or sleeping on your side to keep pressure off the anal area
FAQs
How do I get rid of hemorrhoids?
Over-the-counter medications can quickly relieve symptoms. Most hemorrhoids go away on their own in a few days, but lifestyle changes can help prevent them, like: eating a healthy high-fiber diet, drinking plenty of water, and getting regular exercise.
What do hemorrhoids look like?
Hemorrhoids may look like rubbery lumps. A thrombosed hemorrhoid may look like a dark bluish lump coming out of the anus.
What do hemorrhoids feel like?
Hemorrhoids can feel like hard, tender lumps or an ache or pain in the rectum. They can cause itching and discomfort in the anal area.
Do hemorrhoids go away?
Hemorrhoids can come and go. They usually go away on their own.
How long do hemorrhoids last?
Small hemorrhoids may get better after a few days. Large hemorrhoids or those that protrude out of the anus (prolapsed) may take longer to heal and need help from a doctor.
Do hemorrhoids bleed?
Both internal and external hemorrhoids can bleed. If you notice blood on the toilet paper, in the bowl, or in your stool, you should call your doctor to make sure of the cause.
Are hemorrhoids serious?
Although hemorrhoids are irritating, they are generally not a serious concern. They can affect your quality of life, however. If your hemorrhoids are painful, bleeding, or not improving, it’s important to call your doctor.
Is it safe to push hemorrhoids back in?
A prolapsed hemorrhoid will usually shrink and go back inside your rectum on its own. It is safe to carefully push it back into your rectum if needed.
Are hemorrhoids cancerous?
No, hemorrhoids are not cancerous and do not cause cancer. Bleeding from the rectum can be a sign of hemorrhoids or of another condition, like peptic ulcers or cancer, so it’s important to tell your doctor about any rectal bleeding.
Don’t let hemorrhoids cause you discomfort any longer – schedule an appointment today!
Request Appointment



