Patient Education
Crohn’s Disease
What is Crohn’s Disease?
Crohn’s disease is an autoimmune disease that affects the intestine (bowel). In patients with Crohn’s disease, the bowel becomes inflamed, which can cause fatigue, diarrhea, abdominal pain, and other symptoms.
Crohn’s is considered an inflammatory bowel disease (IBD), along with ulcerative colitis. When the inflammatory process isn’t controlled, it can lead to chronic inflammation, thickening of intestinal walls, ulcers, and noticeable symptoms.
Even though Crohn’s disease most often affects the last part of the small intestine, it can affect any part of the gastrointestinal (GI) tract from the mouth to the anus. It can also cause symptoms outside the GI tract, including the eyes, skin, and joints.
There is no cure for Crohn’s disease, but some treatments can significantly reduce symptoms. This allows many with Crohn’s disease to live symptom-free for long periods.
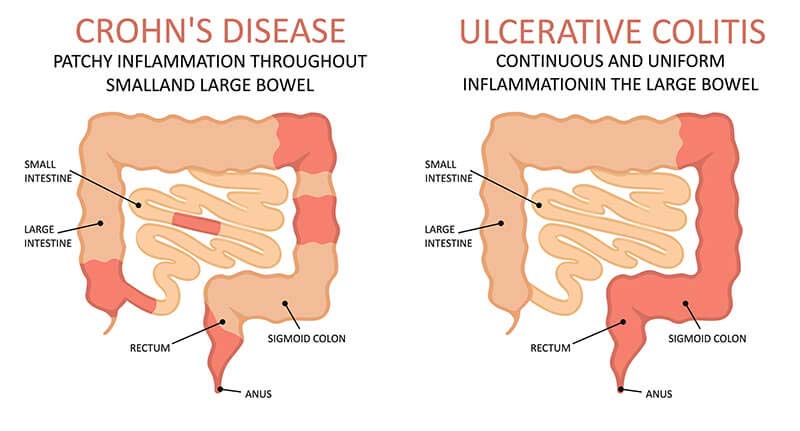
Crohn’s Disease Symptoms
Crohn’s disease can affect different parts of the digestive tract for each patient. The most common areas are the ileum and the colon. The ileum is the last part of the small intestine, and the colon is the last part of the large intestine.
Symptoms of Crohn’s disease can vary from patient to patient and can be mild to severe. They can also worsen over time. Symptoms often come on gradually but can develop quickly without warning in some patients. Some may experience extended periods of time without symptoms. This is known as remission.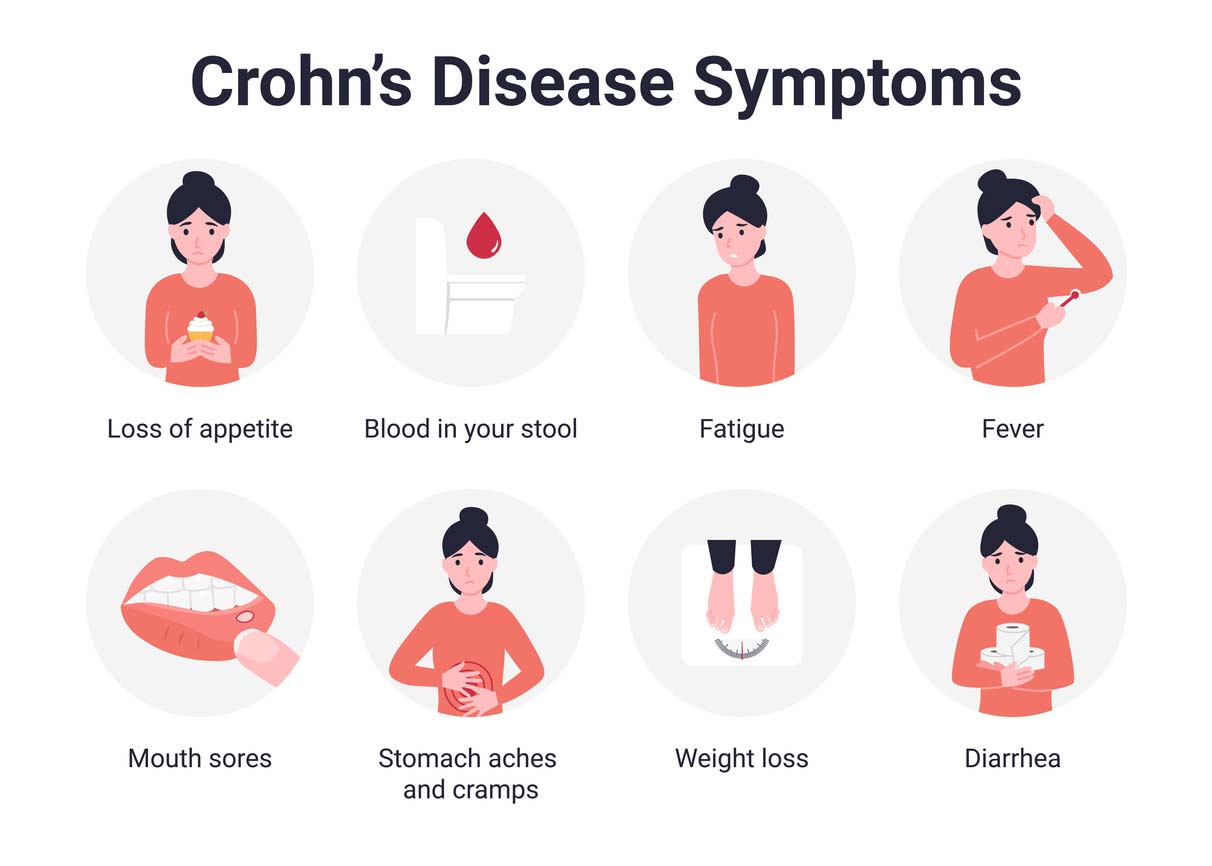
Symptoms of Crohn’s disease may include:
- Abdominal pain / cramping
- Appetite or weight loss
- Bloody stools
- Constipation
- Diarrhea
- Fatigue
- Fever
- Menstrual cycle changes
- Mouth sores
- Night sweats
- Pain, discharge, or bleeding from the rectum
- Urgent need to have a bowel movement
In severe cases, Crohn’s disease symptoms may include:
- Delayed growth and puberty in children
- Eye, skin, or joint inflammation
- Inflammation of the liver or bile ducts
Crohn’s Disease Causes
The exact cause of Crohn’s disease is unknown, but we do know that it’s an immune system response that may be triggered by environmental factors. Crohn’s affects men and women equally and is most commonly diagnosed between the ages of 15 and 35.
It also tends to run in families and affects certain groups more than others, suggesting that genetic factors are important. However, many people with Crohn’s disease do not have a family history. But having a family history of Crohn’s doesn’t guarantee that you’ll develop it.
Crohn’s is not contagious, and it’s not caused by anything you did, ate, or drank. It’s also not caused by stress, although stress can trigger flares (times when you are experiencing symptoms).
Crohn’s Disease Diagnosis
The signs and symptoms of Crohn’s disease are similar to more common illnesses. Your doctor will only diagnose Crohn’s disease after ruling out other causes of your symptoms. Because there is no single test for Crohn’s disease, your doctor will use a combination of tests and procedures to confirm the diagnosis.
If you are diagnosed with Crohn’s, routine testing will become an essential part of managing your condition.
Tests commonly used to diagnose Crohn’s include:
Blood and Stool Tests
Both blood and stool tests give you and your doctor important clues about your condition.
- Blood tests can show anemia, infection, vitamin and mineral deficiencies, and specific indicators of inflammation.
- Stool samples can be tested for certain indicators of inflammation and pathogenic bacteria.
Imaging Tests
Imaging tests can show your doctor areas where there is disease activity and possible complications. Some standard tests used for Crohn’s include:
- Capsule Endoscopy – A tiny wireless camera travels through your digestive tract and takes pictures. The capsule is similar in size to a vitamin and is swallowed. As the capsule works its way through the digestive tract, thousands of images are transmitted to a recorder you wear around your waist. Your doctor will then look for signs of Crohn’s disease in the images.
- CT Scan – A special type of X-ray that takes pictures from different angles at the same time, creating a cross-sectional picture of your bowel. A CT scan allows the doctor to inspect the entire bowel and surrounding tissues to help determine the location and extent of your Crohn’s.
- Endoscopy – This test uses a long flexible tube with a camera to view inside your GI tract. A sigmoidoscopy examines the lower part of the large intestine, while a colonoscopy focuses on the entire colon. Small tissue samples (biopsies) may be removed for further testing. If small bunches of inflamed tissue (granulomas) are present, it can help confirm a Crohn’s diagnosis. An endoscopy can be combined with ultrasound for additional imaging (endoscopic ultrasound).
- Leukocyte Scintigraphy (White Blood Cell Scan) – This test is used to determine how much inflammation is in your GI tract. It tracks white blood cells, which gather at the site of inflammation.
- MRI – Magnetic Resonance Imaging uses a powerful magnet to create detailed images of the bowel and surrounding tissues and organs. MRI is helpful in evaluating fistulas in the small intestine or anal area.
- X-rays – With an X-ray, your doctor can see if there is narrowing, widening, blockages, or developing perforations of the intestines.
Crohn’s Disease Treatment
The main goals of Crohn’s disease treatment are to manage symptoms, achieve remission (no symptoms), prevent flares, and control the inflammation.
Treatment of Crohn’s disease will vary depending on the location of the disease and the severity. Crohn’s can go into remission on its own, making it difficult to know for sure if a particular treatment is working.
Over time, treatment can help improve long-term prognosis by reducing the chances of complications.
Every person’s treatment is different, based on individual factors, like:
- Location in the GI tract
- Medication side effects
- Past responses to treatment
- Severity of the disease
- Your other medical conditions
Anti-inflammatory Medications
Medications are usually the first step in inflammatory bowel disease treatment. Anti-inflammatory medications are meant to suppress the abnormal immune system inflammatory response that causes symptoms.
Doctors may prescribe one or more of the following:
- Aminosalicylates (5-ASAS) – These medications decrease inflammation in the intestinal wall. They’re typically more effective for ulcerative colitis.
- Antibiotics – Antibiotics are given when infections are present.
- Biologic therapies – Biologics work by targeting certain proteins that contribute to inflammation, or by keeping white blood cells from reaching inflamed tissues.
- Corticosteroids – These help keep the immune system from starting or maintaining an inflammatory response.
- Immunomodulators – These drugs change how the immune system works, stopping it from causing inflammation.
Over-the-Counter Medications
Over-the-counter medications can also be used to relieve symptoms, with your doctor’s approval, including antidiarrheals, pain relievers, vitamin and mineral supplements.
Surgery
Surgery is often seen as a last resort since medical treatment often controls the symptoms and complications of Crohn’s. Surgery does not cure the disease, but it may be the fastest way to restore health in some patients. It’s used most often to close fistulas, bypass obstructions, stop bleeding, or remove part of the intestine.
There are different types of surgery to treat different locations in the GI tract and complications, including:
- Fistula removal – Inflammation can cause ulcers in the intestines that can tunnel through the intestinal wall, draining pus. These are called fistulas. They can be treated with medication, surgery, or both.
- Strictureplasty – Inflammation can cause a narrowing (stricture) of part of the intestine, which can contribute to an intestinal blockage. A structuralist widens the narrowed section.
- Small or large bowel resection – Damaged portions of the small or large intestine can be removed via resection. The healthy ends are then joined together.
- Proctocolectomy and Colectomy – In very severe cases, the colon or rectum may be removed. A proctocolectomy removes the colon and rectum and creates a stoma to remove waste out of the body. A colectomy removes the colon but attaches the small intestine to the rectum so waste may still be passed through the anus.
Even though it’s not a cure, surgery can improve the health and wellbeing of patients. Over 85% of patients have no symptoms in the year following surgery. Up to 20% of patients have no symptoms 15 years after surgery.
The chance of recurrence of symptoms after surgery is high, but the use of medication after surgery can decrease that risk.
Lifestyle Changes
Maintaining a healthy lifestyle can help reduce the symptoms of Crohn’s disease and extend the period between flare-ups. It’s important to maintain a healthy lifestyle even when Crohn’s disease is in remission.
The lifestyle changes that make the biggest impact are exercising regularly, eating a healthy diet, and quitting smoking. Reducing stress can also help prevent flares.
Stress doesn’t cause Crohn’s disease, but it can make symptoms worse and can trigger flares. It’s not possible to avoid all stress, but there are ways to help manage it, including:
- Exercise – Even mild physical activity can help reduce stress and depression, and aid digestion and bowel function. Your doctor can help recommend what exercise is most appropriate for you.
- Relaxation, breathing exercises, or meditation – Relaxation techniques like deep, slow breathing can decrease stress and anxiety. Instructional videos on meditation, breathing exercises, yoga, Tai Chi, and other stress management techniques can be found for free online, or you may find local classes.
- Hobbies and activities – Activities that bring you joy like art, gardening, or other hobbies can help you relieve stress.
- Connection – Spending time with friends or family counteracts stress responses and helps prevent depression and anxiety.
Crohn’s Disease Diet
The foods you eat aren’t believed to cause inflammatory bowel disease, but some foods and beverages may aggravate your symptoms. And the symptoms of Crohn’s can make it difficult to get proper nutrition, leading to weight loss, malnutrition, and nutrient deficiencies.
You may consider creating a food diary to keep track of your diet and how you feel. Some foods may cause symptoms to flare up, and tracking can make it easier to identify those foods and eliminate them.
There is no single diet for Crohn’s because every person’s experience with Crohn’s is different. But there are some general recommendations:
- Avoid problem foods – Caffeine, alcohol, and spicy foods may make symptoms worse.
- Reduce dairy – Many people with Crohn’s find that abdominal pain, gas, and diarrhea are decreased when they limit or eliminate dairy products. This could be a sign of lactose intolerance, which means your body has trouble digesting the sugar in dairy products (lactose).
- Avoid high-fat foods – Those with Crohn’s disease in the small intestines may not digest fat normally. Instead of absorbing fat, it passes through your system, worsening diarrhea. Fried foods, cream sauces, and butter all have high-fat content.
- Limit fiber (if necessary) – Fresh fruits, vegetables, and whole grains are part of a healthy diet but can cause discomfort in some people with inflammatory bowel disease. Steaming or baking vegetables may help reduce symptoms.
- Avoid large meals – Some patients find eating five to six smaller meals a day makes them feel better than eating the traditional two or three times a day.
- Drink more water – Fluids are an essential part of digestion, and water is the best choice.
- Visit a dietitian – If your diet is too limited or you lose weight unintentionally, visit with a registered dietitian. GCSA has a registered dietitian on staff – learn more.
Crohn’s Disease Complications
Crohn’s disease can lead to severe complications. Untreated, the chronic inflammation caused by Crohn’s can lead to dangerous, fatal complications.
Some of the potential complications of Crohn’s disease include:
- Abscess – A cavity or hole filled with infected fluid.
- Anemia – Low iron in the blood due to loss of blood in the stool or lack of nutrients.
- Bone loss (osteopenia or osteoporosis) – Lack of nutrients and steroid use contribute to bone loss.
- Bowel obstruction – Inflammation can cause parts of the intestine to narrow, interfering with digestion.
- Colitis – Inflammation of the colon.
- Colorectal cancer
- Eye inflammation
- Fissures – Painful tears in the anus that can bleed.
- Fistula – A tunnel or hole in the intestine that drains pus, caused by inflammation.
- Gallstones – Crohn’s can affect your ability to metabolize bilirubin, increasing the
- risk of gallstones.
- Ileitis – Long-term inflammation of the lower part of the small intestine.
- Ileocolitis – Inflammation of the end of the small intestine and the large intestine (colon).
- Liver Inflammation
- Malnutrition – Caused by vitamin and mineral deficiencies when the intestine is too damaged to adequately absorb nutrients.
- Mouth sores
- Perianal complications (fissures, ulceration, fistulas, abscesses, stenosis)
- Skin conditions
Living With Crohn’s Disease
Crohn’s disease can be very challenging to live with. It can affect your body’s ability to absorb the nutrients you need to stay healthy. The symptoms can interrupt your day-to-day life, making you miss out on special occasions, work, or school. And if left untreated, Crohn’s can be dangerous.
Even so, many people live active lives with Crohn’s, with the right treatment. Getting treatment is essential. Crohn’s is a chronic disease – meaning you’ll have it for life – and there is no cure yet. But working with your doctor and following your treatment plan carefully may help you keep your disease under your control.
FAQs
How do you get Crohn’s disease?
How you get Crohn’s disease is currently unknown. Many factors may lead to getting Crohn’s disease, including environmental factors and possibly genetics.
Is Crohn’s disease genetic?
Crohn’s disease may be genetic. It does tend to run in families, but having a family member that has Crohn’s disease doesn’t mean you will get it. And, you can still have Crohn’s disease with no family history.
Is Crohn’s disease fatal?
Crohn’s disease is usually not fatal. With the help of a doctor, most people are able to keep their Crohn’s disease under control. However, if Chrohn’s disease is left untreated, there can be fatal complications.
How to you spell Crohn’s disease?
The correct spelling is Crohn’s disease, as it is named after Dr. Burrill B. Crohn. A common mispelling is Chrons disease.
Clinical Trials
For clinical trials in Crohn’s disease, please visit www.clinicaltrials.gov.
Crohn’s Disease Testimonial
“Dr. Arnold is a wonderful gastroenterologist (I have Crohn’s, and have been to many docs in the U.S. and abroad to compare him to). It’s easy to get appointments. The staff is friendly, professional, and welcoming. I am always seen on time; the nurses and doctor are never rushed and have patience for questions, explaining and discussing things with me as an equal (not talking down to patients, like some healthcare folks do these days). I highly recommend GCSA.” – Sr. O’Connor



